Coding and Billing for Mental Health Services in USA: Complete Guide for Accurate Claims and Faster Payments
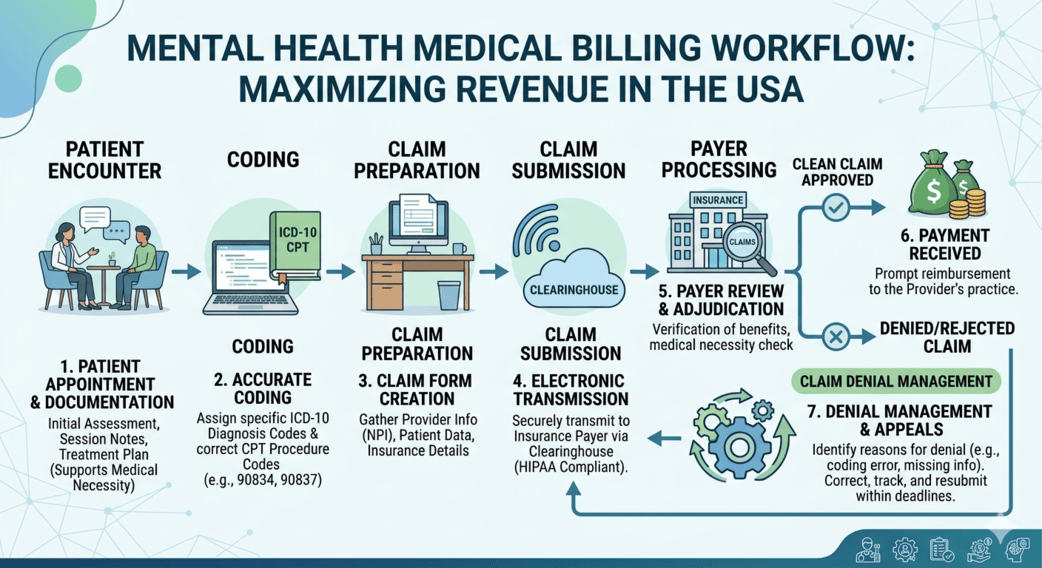
Mental health practices across the United States face a unique mix of clinical responsibility and administrative complexity. From therapy sessions to psychiatric evaluations, every service must be documented, coded, and billed correctly to ensure steady revenue and compliance. This is where coding and billing for mental health services becomes a critical function, not just a backend task.
Whether you are an independent therapist, a growing clinic, or a large behavioral health organization, understanding how billing works can directly impact your reimbursements, denials, and overall financial health.
Key Points You Should Know
- Accurate coding ensures proper reimbursement and reduces claim denials
- Documentation supports medical necessity and compliance
- Payer-specific rules differ, especially for billing Medicare for mental health services
- Outsourcing can improve efficiency and reduce administrative burden
- Credentialing plays a major role in claim approval and provider legitimacy
Understanding Coding and Billing for Mental Health Services
At its core, coding and billing for mental health services involves translating clinical sessions into standardized codes that insurance companies understand. These codes include CPT, ICD-10, and HCPCS codes, each representing diagnoses, procedures, and services provided.
For example, psychotherapy sessions, medication management, and group therapy all have specific codes. Using the wrong code or mismatching it with documentation can lead to delays or denials.
Mental health providers must also ensure that their documentation clearly reflects the services rendered. This includes session duration, treatment goals, progress notes, and clinical justification.
Why Billing for Mental Health Providers Is More Complex
Unlike other medical specialties, billing for mental health providers often involves time-based services, varying session types, and strict documentation requirements.
Some key challenges include:
- Time-based CPT coding for therapy sessions
- Telehealth billing regulations
- Insurance limitations on session frequency
- Prior authorization requirements
- Coordination between primary and secondary insurance
Because of these factors, billing for mental health services requires a deeper understanding of payer policies and compliance rules.
Common Codes Used in Mental Health Billing
Medical billing for mental health relies heavily on CPT codes for therapy and psychiatric services. Some commonly used categories include:
- Psychiatric diagnostic evaluation
- Individual psychotherapy
- Family or group therapy
- Medication management
- Crisis intervention
Each code must align with the diagnosis and documentation. Mental health medical billing professionals must stay updated with coding changes to avoid revenue leakage.
The Role of Documentation in Mental Health Billing
Documentation is the backbone of successful billing for mental health. Without proper notes, even correctly coded claims can be denied.
Essential documentation elements include:
- Patient history and diagnosis
- Treatment plan
- Session notes with time duration
- Progress tracking
- Medical necessity justification
Strong documentation not only supports billing but also protects providers during audits.
Billing Medicare for Mental Health Services
Billing Medicare for mental health services comes with its own set of guidelines. Medicare typically covers services such as individual therapy, group therapy, and psychiatric evaluations, but only under specific conditions.
Providers must ensure:
- The patient meets medical necessity criteria
- Services are provided by credentialed professionals
- Documentation aligns with Medicare requirements
- Correct modifiers and place of service codes are used
Failure to comply with these rules can result in claim rejections or audits.
In-House vs Outsourcing Mental Health Billing
Many practices struggle with whether to manage billing internally or opt for outsourcing mental health billing.
In-house billing offers control but comes with challenges such as staffing costs, training, and error risks. On the other hand, outsourced billing for mental health provides access to experienced professionals who specialize in behavioral and mental health billing services.
Benefits of outsourcing include:
- Reduced administrative workload
- Faster claim submission and follow-ups
- Improved accuracy and reduced denials
- Access to advanced billing software
Choosing the best outsource mental health billing and coding services can significantly improve your revenue cycle.
How Mental Health Billing Solutions Improve Efficiency
Modern mental health billing solutions are designed to streamline the entire revenue cycle. These systems integrate scheduling, documentation, coding, and claim submission into a single workflow.
Features often include:
- Automated claim scrubbing
- Real-time eligibility verification
- Denial management tools
- Reporting and analytics
Such solutions help practices maintain consistency in billing mental health services while reducing manual errors.
Importance of Credentialing in Mental Health Billing
Credentialing is often overlooked but plays a crucial role in mental health billing and credentialing services. Without proper credentialing, insurance companies will not reimburse providers.
The credentialing process includes:
- Verifying provider qualifications
- Enrolling with insurance networks
- Maintaining updated provider information
Delays in credentialing can lead to revenue loss, making it essential for practices to manage this process efficiently.
Challenges Faced by Mental Health Clinics
Billing services for mental health clinics must address several ongoing challenges:
- High claim denial rates
- Frequent policy changes by insurers
- Complex coding requirements
- Managing multiple payer rules
A cheap outsource mental health billing company might seem attractive, but quality and expertise should always be the priority.
Best Practices for Billing Services for Mental Health
To ensure smooth operations and consistent revenue, follow these best practices:
- Verify insurance eligibility before every session
- Use accurate and updated CPT and ICD codes
- Maintain detailed and compliant documentation
- Monitor claims and follow up on denials
- Regularly audit billing processes
These steps can significantly improve the efficiency of billing services for mental health providers.
The Future of Mental Health Billing
With increasing demand for mental health services, the billing landscape is evolving rapidly. Telehealth, digital therapy platforms, and integrated care models are reshaping how billing for mental health services is managed.
Practices that adopt advanced mental health billing services and stay updated with regulatory changes will have a competitive advantage.
How Professional Billing Support Can Help
Partnering with an experienced provider offering behavioral and mental health billing services ensures that your practice stays compliant while maximizing revenue.
At the end of the day, mental health professionals should focus on patient care, not administrative stress. This is where a reliable partner like 247 Medical Billing Services can support your growth through comprehensive medical billing services, medical coding services, medical billing and coding services, revenue cycle management services, and credentialing services, all tailored to the needs of mental health practices.
Conclusion
Coding and billing for mental health services is more than just submitting claims. It is a structured process that requires accuracy, compliance, and continuous monitoring. From understanding codes to managing documentation and payer rules, every step plays a role in your financial success.
By adopting the right strategies, leveraging mental health billing solutions, and considering outsourcing when needed, providers can reduce errors, improve reimbursements, and focus on delivering quality care.
FAQs
What is coding and billing for mental health services?
It involves assigning standardized codes to mental health treatments and submitting claims to insurance companies for reimbursement.
Why is mental health billing different from other medical billing?
It often includes time-based coding, complex documentation, and varying payer requirements, making it more detailed and specialized.
Can I handle billing for mental health services in-house?
Yes, but it requires trained staff, updated knowledge, and proper systems. Many providers choose outsourcing for better efficiency.
What are common mistakes in mental health billing?
Incorrect coding, poor documentation, missing modifiers, and failure to verify insurance eligibility are common issues.
How does outsourcing mental health billing help?
It reduces administrative burden, improves accuracy, speeds up reimbursements, and allows providers to focus on patient care.
What is the role of credentialing in mental health billing?
Credentialing ensures providers are authorized by insurance companies, which is necessary for receiving payments.
Are mental health services covered by Medicare?
Yes, but providers must follow strict guidelines and ensure proper documentation and coding for successful claims.
- Art
- Causes
- Crafts
- Dance
- Drinks
- Film
- Fitness
- Food
- Oyunlar
- Gardening
- Health
- Home
- Literature
- Music
- Networking
- Other
- Party
- Religion
- Shopping
- Sports
- Theater
- Wellness

